- Introduction
- Prostate Cancer
- The Prostate
- Understanding Cancer
- Risk Factors
- Screening
- Symptom
- Diagnosis
- Staging
- Treatment
- Complementary and Alternative
Medicine - Nutrition and Physical Activity
- Follow-up Care
- Sources of Support
- The Promise of Cancer Research
- National Cancer Institute Information
Resources
Introduction
Prostate cancer is the second most common type of cancer among men in this country. Only skin cancer is more common. Out of every three men who are diagnosed with cancer each year, one is diagnosed with prostate cancer. Yet when detected early, the relative five year survival rate is nearly 100%!
You will read about possible causes, screening, symptoms, diagnosis, and treatment. You will also find ideas about how to cope with the disease.
Scientists are studying prostate cancer to find out more about its causes. And they are looking for better ways to treat it.
Prostate Cancer
Definition of prostate cancer: Cancer that forms in tissues of the prostate (a gland in the male reproductive system found below the bladder and in front of the rectum). Prostate cancer usually occurs in older men.
Estimated new cases and deaths from prostate cancer in the United States in 2008:
New cases: 186,320
Deaths: 28,660
The Prostate
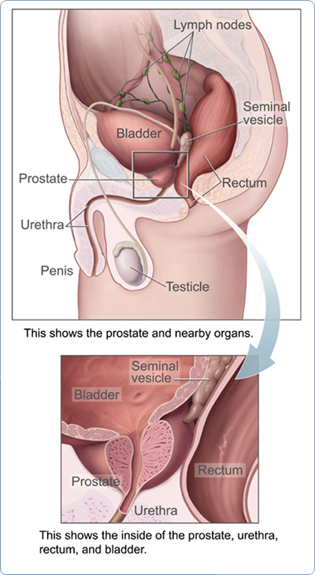
The prostate is part of a man's reproductive system. It is located in front of the rectum and under the bladder. It surrounds the urethra, the tube through which urine flows. A healthy prostate is about the size of a walnut.
The prostate makes part of seminal fluid. During ejaculation, seminal fluid helps carry sperm out of the man's body as part of semen.
Male hormones (androgens) make the prostate grow. The testicles are the main source of male hormones, including testosterone. The adrenal gland also makes testosterone, but in small amounts.
If the prostate grows too large, it squeezes the urethra. This may slow or stop the flow of urine from the bladder to the penis.
Under standing Cancer
Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body.
Normally, cells grow and divide to form new cells as the body needs them. When cells grow old, they die, and new cells take their place.
Sometimes, this orderly process goes wrong. New cells form when the body does not need them, and old cells do not die when they should. These extra cells can form a mass of tissue called a growth or tumor.
Tumors can be benign or malignant:
- Benign tumors are not cancer:
- Benign tumors are rarely life-threatening.
- Generally, benign tumors can be removed. They usually do not grow back.
- Cells from benign tumors do not invade the tissues around them.
- Cells from benign tumors do not spread to other parts of the body.

Benign prostatic hyperplasia (BPH) is the abnormal growth of benign prostate cells. The prostate grows larger and squeezes the urethra. This prevents the normal flow of urine.
BPH is a very common problem. In the United States, most men over the age of 50 have symptoms of BPH. For some men, symptoms may be severe enough to need treatment.

Malignant tumors are cancer:
- Malignant tumors are generally more serious than benign tumors. They may be life-threatening.
- Malignant tumors often can be removed. But sometimes they grow back.
- Cells from malignant tumors can invade and damage nearby tissues and organs.
- Cells from malignant tumors can spread (metastasize) to other parts of the body. Cancer cells spread by breaking away from the original (primary) tumor and entering the bloodstream or lymphatic system. The cells invade other organs and form new tumors that damage these organs. The spread of cancer is called metastasis.
When prostate cancer spreads, cancer is often found in nearby lymph nodes. If cancer has reached these nodes, it also may have spread to other lymph nodes, the bones, or other organs.
When cancer spreads from its original place to another part of the body, the new tumor has the same kind of abnormal cells and the same name as the primary tumor. For example, if prostate cancer spreads to bones, the cancer cells in the bones are actually prostate cancer cells. The disease is metastatic prostate cancer, not bone cancer. For that reason, it is treated as prostate cancer, not bone cancer. Doctors call the new tumor "distant" or metastatic disease.
Symptoms of BPH: An indication that a person has a condition or disease. Some examples of symptoms are headache, fever, fatigue, nausea, vomiting, and pain.
Metastasize: To spread from one part of the body to another. When cancer cells metastasize and form secondary tumors, the cells in the metastatic tumor are like those in the original (primary) tumor.
Risk Factors
No one knows the exact causes of prostate cancer. Doctors often cannot explain why one man develops prostate cancer and another does not. However, we do know that prostate cancer is not contagious. You cannot "catch" it from another person.
Research has shown that men with certain risk factors are more likely than others to develop prostate cancer. A risk factor is something that may increase the chance of developing a disease.
Studies have found the following risk factors for prostate cancer:
- Age: Age is the main risk factor for prostate cancer. This disease is rare in men younger than 45. The chance of getting it goes up sharply as a man gets older. In the United States, most men with prostate cancer are older than 65.
- Family history: A man's risk is higher if his father or brother had prostate cancer.
- Race: Prostate cancer is more common in African American men than in white men, including Hispanic white men. It is less common in Asian and American Indian men.
- Certain prostate changes: Men with cells called high-grade prostatic intraepithelial neoplasia (PIN) may be at increased risk for prostate cancer. These prostate cells look abnormal under a microscope.
- Diet: Some studies suggest that men who eat a diet high in animal fat or meat may be at increased risk for prostate cancer. Men who eat a diet rich in fruits and vegetables may have a lower risk.
Many of these risk factors can be avoided. Others, such as family history, cannot be avoided. You can help protect yourself by staying away from known risk factors whenever possible.
Scientists have also studied whether BPH, obesity, smoking, a virus passed through sex, or lack of exercise might increase the risk for prostate cancer. At this time, these are not clear risk factors. Also, most studies have not found an increased risk of prostate cancer for men who have had a vasectomy. A vasectomy is surgery to cut or tie off the tubes that carry sperm out of the testicles.
Most men who have known risk factors do not get prostate cancer. On the other hand, men who do get the disease often have no known risk factors, except for growing older.
If you think you may be at risk, you should talk with your doctor. Your doctor may be able to suggest ways to reduce your risk and can plan a schedule for checkups.
Risk Factors: Something that may increase the chance of developing a disease. Some examples of risk factors for cancer include age, a family history of certain cancers, use of tobacco products, certain eating habits, obesity, lack of exercise, exposure to radiation or other cancer-causing agents, and certain genetic changes.
Screening
Your doctor can check you for prostate cancer before you have any symptoms. Screening can help doctors find and treat cancer early. But studies so far have not shown that screening tests reduce the number of deaths from prostate cancer. You may want to talk with your doctor about the possible benefits and harms of being screened. The decision to be screened, like many other medical decisions, is a personal one. You should decide after learning the pros and cons of screening.
Your doctor can explain more about these tests:
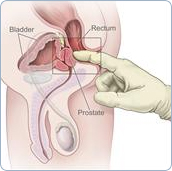
- Digital rectal exam: The doctor inserts a lubricated, gloved finger into the rectum and feels the prostate through the rectal wall. The prostate is checked for hard or lumpy areas.
- Blood test for prostate-specific antigen (PSA): A lab checks the level of PSA in a man's blood sample. A high PSA level is commonly caused by BPH or prostatitis (inflammation of the prostate). Prostate cancer may also cause a high PSA level.
The digital rectal exam and PSA test can detect a problem in the prostate. They cannot show whether the problem is cancer or a less serious condition. Your doctor will use the results of these tests to help decide whether to check further for signs of cancer. Information about other tests is in the "Diagnosis" section.
Screening: Checking for disease when there are no symptoms. Since screening may find diseases at an early stage, there may be a better chance of curing the disease. Examples of cancer screening tests are the mammogram (breast), colonoscopy (colon), Pap smear (cervix), and PSA blood level and digital rectal exam (prostate). Screening can also include checking for a person’s risk of developing an inherited disease by doing a genetic test.
Digital rectal exam: DRE. An examination in which a doctor inserts a lubricated, gloved finger into the rectum to feel for abnormalities. Also called DRE.
PSA. A substance produced by the prostate that may be found in an increased amount in the blood of men who have prostate cancer, benign prostatic hyperplasia, or infection or inflammation of the prostate.
Symptom
A man with prostate cancer may not have any symptoms. For men who have symptoms of prostate cancer, common symptoms include:
» Urinary problems
- Not being able to urinate
- Having a hard time starting or stopping the urine flow
- Needing to urinate often, especially at night
- Weak flow of urine
- Urine flow that starts and stops
- Pain or burning during urination
Most often, these symptoms are not due to cancer. BPH, an infection, or another health problem may cause them. Any man with these symptoms should tell his doctor so that problems can be diagnosed and treated as early as possible. He may see his regular doctor or a urologist. A urologist is a doctor whose specialty is diseases of the urinary system.
Diagnosis
If you have a symptom or test result that suggests cancer, your doctor must find out whether it is due to cancer or to some other cause. Your doctor will ask about your personal and family medical history. You will have a physical exam. You may have lab tests. Your visit may include a digital rectal exam, a urine test to check for blood or infection, and a blood test to measure PSA level.
You also may have other exams:
Transrectal ultrasound: The doctor inserts a probe into the man's rectum to check for abnormal areas. The probe sends out sound waves that people cannot hear (ultrasound). The waves bounce off the prostate. A computer uses the echoes to create a picture called a sonogram.
Cystoscopy: The doctor uses a thin, lighted tube to look into the urethra and bladder.
Transrectal biopsy: A biopsy is the removal of tissue to look for cancer cells. It is the only sure way to diagnose prostate cancer. The doctor inserts a needle through the rectum into the prostate. The doctor takes small tissue samples from many areas of the prostate. Ultrasound may be used to guide the needle. A pathologist checks for cancer cells in the tissue.

You may want to ask the doctor these questions before having a biopsy:
- Where will the biopsy take place? Will I have to go to the hospital?
- How long will it take? Will I be awake? Will it hurt?
- What are the risks? What are the chances of infection or bleeding after the biopsy?
- How long will it take me to recover?
- How soon will I know the results?
If I do have cancer, who will talk to me about the next steps? When?

If Cancer Is Not Found
If the physical exam and test results do not suggest cancer, your doctor may suggest medicine to reduce symptoms caused by an enlarged prostate. Surgery also can relieve these symptoms. The surgery most often used in such cases is transurethral resection of the prostate (TURP or TUR). In TURP, an instrument is inserted through the urethra to remove prostate tissue that is pressing against the upper part of the urethra and restricting the flow of urine. You should talk to your doctor about the best treatment option.
If Cancer Is Found
If cancer is present, the pathologist studies tissue samples from the prostate under a microscope to report the grade of the tumor. The grade tells how much the tumor tissue differs from normal prostate tissue. It suggests how fast the tumor is likely to grow. Tumors with higher grades tend to grow faster than those with lower grades. They are also more likely to spread.
One system of grading prostate cancer uses G1 through G4. Another way of grading is with the Gleason score. The pathologist gives each area of cancer a grade of 1 through 5. The pathologist adds the two most common grades together to make a Gleason score. Or the pathologist may add the most common grade and the highest (most abnormal) grade to get the score. Gleason scores can range from 2 to 10.
Staging
To plan your treatment, your doctor needs to know the extent (stage) of the disease. The stage is based on the size of the tumor, whether the cancer has spread outside the prostate and, if so, where it has spread.
You may have blood tests to see if the cancer has spread. Some men also may need imaging tests:
- Bone scan: The doctor injects a small amount of a radioactive substance into a blood vessel. It travels through the bloodstream and collects in the bones. A machine called a scanner detects and measures the radiation. The scanner makes pictures of the bones on a computer screen or on film. The pictures may show cancer that has spread to the bones.
- CT scan: An x-ray machine linked to a computer takes a series of detailed pictures of areas inside your body. Doctors often use CT scans to see the pelvis or abdomen.
- MRI: A strong magnet linked to a computer is used to make detailed pictures of areas inside your body.
These are the stages of prostate cancer:
- Stage I: The cancer cannot be felt during a digital rectal exam. It is found by chance when surgery is done for another reason, usually for BPH. The cancer is only in the prostate.
- Stage II: The cancer is more advanced, but it has not spread outside the prostate.
- Stage III: The cancer has spread outside the prostate. It may be in the seminal vesicles. It has not spread to the lymph nodes.
- Stage IV: The cancer may be in nearby muscles and organs (beyond the seminal vesicles). It may have spread to the lymph nodes. It may have spread to other parts of the body.
- Recurrent cancer is cancer that has come back (recurred) after a time when it could not be detected. It may recur in or near the prostate. Or it may recur in any other part of the body, such as the bones.
Seminal vesicles: A gland that helps produce semen.
Treatment
» Getting a Second Opinion
» Treatment Methods
Many men with prostate cancer want to take an active part in making decisions about their care. It is natural to want to learn all you can about prostate cancer and your treatment choices. However, shock and stress after the diagnosis can make it hard to think of everything you want to ask your doctor. It often helps to make a list of questions before an appointment.
To help remember what the doctor says, you may take notes or ask whether you may use a tape recorder. You may also want to have a family member or friend with you when you talk to the doctor - to take part in the discussion, to take notes, or just to listen.
You do not need to ask all your questions at once. You will have other chances to ask your doctor or nurse to explain things that are not clear and to ask for more details.
Your doctor may refer you to a specialist, or you may ask for a referral. Specialists who treat prostate cancer include urologists, urologic oncologists, medical oncologists, and radiation oncologists.
Getting a Second Opinion
Before starting treatment, you might want a second opinion about your diagnosis and treatment plan. Many insurance companies cover a second opinion if you or your doctor requests it. It may take some time and effort to gather medical records and arrange to see another doctor. Usually it is not a problem to take several weeks to get a second opinion. In most cases, the delay in starting treatment will not make treatment less effective. To make sure, you should discuss this delay with your doctor. Some men with prostate cancer need treatment right away.
There are a number of ways to find a doctor for a second opinion:
- Your doctor may refer you to one or more specialists. At cancer centers, several specialists often work together as a team.
- For a list of nearby treatment centers call the National Cancer Institute at 1-800-4-CANCER
- A local or state medical society, a nearby hospital, or a medical school can usually provide the names of specialists.
- The American Board of Medical Specialties (ABMS) has a list of doctors who have had training and passed exams in their specialty. You can find this list in the Official ABMS Directory of Board Certified Medical Specialists. This Directory is in most public libraries. Also, ABMS offers this information at http://www.abms.org. (Click on "Who's Certified.")
Treatment Methods
Men with prostate cancer have many treatment options. The treatment that is best for one man may not be best for another.
Treatment may involve surgery, radiation therapy, or hormone therapy. You may have a combination of treatments. If your doctor recommends watchful waiting, your health will be monitored closely. You will have treatment only if symptoms occur or get worse.
Cancer treatment is either local therapy or systemic therapy:
- Local therapy: Surgery and radiation therapy are local treatments. They remove or destroy cancer in the prostate. When prostate cancer has spread to other parts of the body, local therapy may be used to control the disease in those specific areas.
- Systemic therapy: Hormone therapy is systemic therapy. Hormones are given to control cancer that has spread.
The treatment that is right for you depends on the stage of the cancer, the grade of the tumor, your symptoms, and your general health. Your doctor will describe your treatment choices and the expected results.
Because cancer treatments often damage healthy cells and tissues, side effects are common. Side effects depend mainly on the type and extent of the treatment. Side effects may not be the same for each man, and they may change from one treatment session to the next.
You should consider both the expected benefits and possible side effects of each treatment option. You may want to discuss with your doctor the possible effects on sexual activity. You can work with your doctor to create a treatment plan that reflects your medical needs and personal values.
At any stage of disease, supportive care is available to control pain and other symptoms, to relieve the side effects of treatment, and to ease emotional concerns.
You may want to talk to your doctor about taking part in a clinical trial, a research study of new treatment methods.

You may want to ask your doctor these questions before your treatment begins:
- What is the stage of the disease? Do any lymph nodes show signs of cancer? Has the cancer spread?
- What is the grade of the tumor?
- What is the goal of treatment? What are my treatment choices? Which do you recommend for me? Why?
- What are the expected benefits of each kind of treatment?
- What are the risks and possible side effects of each treatment? How can side effects be managed?
- What can I do to prepare for treatment?
- Will I need to stay in the hospital? If so, for how long?
- How will treatment affect my normal activities? Will it affect my sex life? Will I have urinary problems? Will I have bowel problems?
- What will the treatment cost? Will my insurance cover it?
- Would a clinical trial (research study) be appropriate for me?

Surgery
Surgery is a common treatment for early stage prostate cancer. Your doctor may remove the whole prostate or only part of it. In some cases, your doctor can use a method known as nerve-sparing surgery. This type of surgery may save the nerves that control erection. But if you have a large tumor or a tumor that is very close to the nerves, you may not be able to have this surgery.
Each type of surgery has benefits and risks. Your doctor can further describe these types:
- Radical retropubic prostatectomy: The doctor removes the entire prostate and nearby lymph nodes through an incision (cut) in the abdomen.
- Radical perineal prostatectomy: The doctor removes the entire prostate through a cut between the scrotum and the anus. Nearby lymph nodes may be removed through a separate cut in the abdomen.
- Laparoscopic prostatectomy: The doctor removes the entire prostate and nearby lymph nodes through small incisions, rather than a single long cut in the abdomen. A thin, lighted tube (a laparoscope) is used to help remove the prostate.
- Transurethral resection of the prostate (TURP): The doctor removes part of the prostate with a long, thin device that is inserted through the urethra. The cancer is cut from the prostate. TURP may not remove all of the cancer. But it can remove tissue that blocks the flow of urine.
- Cryosurgery: This type of surgery for prostate cancer is under study at some medical centers.
- Pelvic lymphadenectomy: This is routinely done during prostatectomy. The doctor removes lymph nodes in the pelvis to see if cancer has spread to them. If there are cancer cells in the lymph nodes, the disease may have spread to other parts of the body. In this case, the doctor may suggest other types of treatment.
The time it takes to heal after surgery is different for each man and depends on the type of surgery he has had. You may be uncomfortable for the first few days. However, medicine can help control the pain. Before surgery, you should discuss the plan for pain relief with your doctor or nurse. After surgery, your doctor can adjust the plan if you need more pain relief.
After surgery, the urethra needs time to heal. You will have a catheter. A catheter is a tube put through the urethra into the bladder to drain urine. You will have the catheter for 5 days to 3 weeks. Your nurse or doctor will show you how to care for it.
Surgery may cause short-term problems, such as incontinence. After surgery, some men may lose control of the flow of urine (urinary incontinence). Most men regain bladder control after a few weeks.
Some men may become impotent. Nerve-sparing surgery is an attempt to avoid the problem of impotence. If a man can have nerve-sparing surgery and the operation is a success, impotence may not last. In some cases, men become permanently impotent. You can talk with your doctor about medicine and other ways to help manage the sexual effects of cancer treatment.
If your prostate is removed, you will no longer produce semen. You will have dry orgasms. If you wish to father children, you may consider sperm banking or a sperm retrieval procedure.

You may want to ask your doctor these questions before choosing surgery:
- What kinds of surgery can I consider? Is nerve-sparing surgery an option for me? Which operation do you recommend for me? Why?
- How will I feel after the operation?
- If I have pain, how can we control it?
- Will I have any lasting side effects?
- Is there someone I can talk with who has had the same surgery I'll be having?

Radiation Therapy
Radiation therapy (also called radiotherapy) uses high-energy rays to kill cancer cells. It affects cells only in the treated area.
For early stage prostate cancer, radiation treatment may be used instead of surgery. It also may be used after surgery to destroy any cancer cells that remain in the area. In later stages of prostate cancer, radiation treatment may be used to help relieve pain.
Doctors use two types of radiation therapy to treat prostate cancer. Some men receive both types:
- External radiation: The radiation comes from a large machine outside the body. Men go to a hospital or clinic for treatment. Treatments are usually 5 days a week for several weeks. Many men receive 3-dimensional conformal radiation therapy. This type of treatment more closely targets the cancer. It spares healthy tissue.
- Internal radiation (implant radiation therapy or brachytherapy): The radiation comes from radioactive material usually contained in small seeds. The seeds are put into the tissue. They give off radiation for months. The seeds are harmless and do not need to be removed.
Side effects depend mainly on the dose and type of radiation. You are likely to be very tired during radiation therapy, especially in the later weeks of treatment. Resting is important, but doctors usually advise patients to try to stay as active as they can.
If you have external radiation, you may have diarrhea or frequent and uncomfortable urination. Some men have lasting bowel or urinary problems. Your skin in the treated area may become red, dry, and tender. You may lose hair in the treated area. The hair may not grow back.
Internal radiation treatment may cause incontinence. This side effect usually goes away. Lasting side effects from internal radiation are not common.
Both internal and external radiation can cause impotence. Internal radiation is less likely to have this effect.

You may want to ask your doctor these questions before choosing radiation therapy:
- How will radiation be given?
- When will treatment start? When will it end? How often will I have treatments?
- What can I do to take care of myself before, during, and after treatment?
- How will I feel during treatment? Will I be able to drive myself to and from treatment?
- How will we know the treatment is working?
- How will I feel after the radiation?
- Are there any lasting effects?
- What is the chance that the cancer will come back in my prostate?
- How often will I need checkups?

Hormone Therapy
Hormone therapy keeps prostate cancer cells from getting the male hormones (androgens) they need to grow. The testicles are the body's main source of the male hormone testosterone. The adrenal gland makes a small amount of testosterone.
Hormone treatment uses drugs or surgery:
- Drugs: Your doctor may suggest a drug that can block natural hormones.
- Luteinizing hormone-releasing hormone (LH-RH) agonists: These drugs can prevent the testicles from making testosterone. Examples are leuprolide and goserelin.
- Antiandrogens: These drugs can block the action of male hormones. Examples are flutamide, bicalutamide, and nilutamide.
- Other drugs: Some drugs can prevent the adrenal gland from making testosterone. Examples are ketoconazole and aminoglutethimide.
- Surgery: Surgery to remove the testicles is called orchiectomy.
After orchiectomy or treatment with an LH-RH agonist, your body no longer gets testosterone from the testicles. However, the adrenal gland still produces a small amount of male hormones. You may receive an antiandrogen to block the action of the male hormones that remain. This combination of treatments is known as total androgen blockade. Studies have not shown whether total androgen blockade is more effective than surgery or an LH-RH agonist alone.
Doctors can usually control prostate cancer that has spread to other parts of the body with hormone therapy. The cancer often does not grow for several years. But in time, most prostate cancers can grow with very little or no male hormones. Hormone therapy is no longer helpful. At that time, your doctor may suggest other forms of treatment that are under study.
Hormone therapy is likely to affect your quality of life. It often causes side effects such as impotence, hot flashes, loss of sexual desire, and weaker bones. An LH-RH agonist may make your symptoms worse for a short time when you first take it. This temporary problem is called "flare." The treatment gradually causes your testosterone level to fall. Without testosterone, tumor growth slows. Your condition may improve. (To prevent flare, your doctor may give you an antiandrogen for a while along with the LH-RH agonist.)
Antiandrogens (such as nilutamide) can cause nausea, diarrhea, or breast growth or tenderness. Rarely, they may cause liver problems (pain in the abdomen, yellow eyes, or dark urine). Some men who use nilutamide may have difficulty breathing. Some may have trouble adjusting to sudden changes in light.
If used for a long time, ketoconazole may cause liver problems, and aminoglutethimide can cause skin rashes. If you receive total androgen blockade, you may have more side effects than if you have just one type of hormone treatment.
Any treatment that lowers hormone levels can weaken your bones. Your doctor can suggest medicines or dietary supplements that can reduce your risk of bone fractures.

You may want to ask your doctor these questions before choosing hormone therapy:
- What kind of hormone therapy will I have? Would you recommend drugs or surgery? Why?
- When will treatment start? How often will I have treatments? When will it end?
- Where will I go for treatment? Will I be able to drive home afterward?
- If I have surgery, how long will I need to stay in the hospital?
- How will I feel during treatment?
- What can I do to take care of myself during treatment?
- How will we know the treatment is working?
- Which side effects should I tell you about?
- Will there be lasting side effects?

Watchful Waiting
You may choose watchful waiting if the risks and possible side effects of treatment outweigh the possible benefits. Your doctor may offer this choice if you are older or have other serious health problems. Your doctor may also suggest watchful waiting if you are diagnosed with early stage prostate cancer that seems to be slowly growing. Your doctor will offer you treatment if symptoms occur or get worse.
Watchful waiting avoids or delays the side effects of surgery and radiation, but this choice has risks. It may reduce the chance to control cancer before it spreads. Also, it may be harder to cope with surgery and radiation therapy as you age.
You may decide against watchful waiting if you do not want to live with an untreated cancer. If you choose watchful waiting but grow concerned later, you should discuss your feelings with your doctor. A different approach is nearly always available.

You may want to ask your doctor these questions before choosing watchful waiting:
- If I choose watchful waiting, can I change my mind later on?
- Will the cancer be harder to treat later?
- How often will I have checkups?
- Between checkups, what problems should I report?

Complementary and Alternative Medicine
Some men with prostate cancer use complementary and alternative medicine (CAM):
- An approach is generally called complementary medicine when it is used along with standard treatment.
- An approach is called alternative medicine when it is used instead of standard treatment.
Acupuncture, massage therapy, herbal products, vitamins or special diets, visualization, meditation, and spiritual healing are types of CAM.
Many men say that CAM helps them feel better. However, some types of CAM may change the way standard treatment works. These changes could be harmful. And some types of CAM could be harmful even if used alone.
Some types of CAM are expensive. Health insurance may not cover the cost.
You also may request materials from the Federal Government's National Center for Complementary and Alternative Medicine. You can reach their clearinghouse toll-free at 1-888-644-6226 (voice) and 1-866-464-3615 (TTY).
CAM: Forms of treatment that are used in addition to (complementary) or instead of (alternative) standard treatments. These practices generally are not considered standard medical approaches. Standard treatments go through a long and careful research process to prove they are safe and effective, but less is known about most types of CAM. CAM may include dietary supplements, mega dose vitamins, herbal preparations, special teas, acupuncture, massage therapy, magnet therapy, spiritual healing, and meditation.
Nutrition and Physical Activity
It is important for men with prostate cancer to take care of themselves. Taking care of yourself includes eating well and staying as active as you can.
You need the right amount of calories to maintain a good weight. You also need enough protein to keep up your strength. Eating well may help you feel better and have more energy. Your doctor, dietitian, or other health care provider can suggest a healthy diet.
Many men find they feel better when they stay active. Walking, yoga, swimming, and other exercise can keep you strong and increase your energy. Exercise may reduce pain and make treatment easier to handle. It also can help relieve stress. Whatever physical activity you choose, be sure to talk to your doctor before you start. Also, if your activity causes you pain or other problems, be sure to let your doctor or nurse know about it.
Your Diet Is an Important Part of Your Treatment
Your diet is an important part of your treatment for cancer. Eating the right kinds of foods before, during, and after your treatment can help you feel better and stay stronger.
A registered dietitian is your best source of information about your diet. The information here will add to what the dietitian can tell you. Feel free to ask for help or advice when you need it. Writing down your questions in advance will help you make sure you get the information you need. Ask the dietitian to repeat or explain anything that is not clear. She or he can also explain anything in this book if you have a question and can give you more detailed information. Your doctor or nurse can also give you helpful advice and can refer you to a registered dietitian. If you cannot get a referral, call the American Dietetic Association's (ADA) toll-free nutrition hotline. The information specialist you talk to can help you find a registered dietitian in your area. The Resources section at the end of Eating Hints provides the telephone number and other contact information for the ADA.
American Dietetic Association (ADA)
The ADA is a professional society of registered dietitians and other professionals working in food- and nutrition-related fields. For a referral to a registered dietitian in your area and to listen to recorded food and nutrition messages, call the ADA's consumer nutrition hotline at 1-800-366-1655. Or, visit the ADA's home page on the World Wide Web at http://www.eatright.org.
Follow-up Care
Follow-up care after treatment for prostate cancer is important. Even when the cancer seems to have been completely removed or destroyed, the disease sometimes returns because undetected cancer cells remained somewhere in the body after treatment. Your doctor will monitor your recovery and check for recurrence of the cancer. Checkups help ensure that any changes in your health are noted and treated if needed. Checkups may include lab tests, x-rays, biopsies, or other tests. Between scheduled visits, you should contact your doctor if you have any health problems.
Facing Forward Series: Life After Cancer Treatment is an NCI booklet for people who have completed their treatment. It answers questions about follow-up care and other concerns. It has tips for making the best use of medical visits. It also suggests ways to talk with your doctor about creating a plan of action for recovery and future health. You May order this booklet free by calling the National Cancer Institute at: 1-800-4-CANCER (1-800-422-6237)
TTY: 1-800-332-8615
Sources of Support
Learning you have prostate cancer can change your life and the lives of those close to you. These changes can be hard to handle. It is normal for you, your family, and your friends to have many different and sometimes confusing feelings.
You may worry about caring for your family, keeping your job, or continuing daily activities. Concerns about treatments and managing side effects, hospital stays, and medical bills are also common. Doctors, nurses, and other members of your health care team can answer questions about treatment, working, or other activities. Meeting with a social worker, counselor, or member of the clergy can be helpful if you want to talk about your feelings or concerns. Often, a social worker can suggest resources for financial aid, transportation, home care, or emotional support.
Friends and relatives can be supportive. Support groups also can help. In these groups, patients or their family members meet with other patients or their families to share what they have learned about coping with the disease and the effects of treatment. Groups may offer support in person, over the telephone, or online. You may want to talk with a member of your health care team about finding a support group.
You and your partner may be concerned about the effects of prostate cancer on your sexual relationship. You may want to talk with your doctor about possible treatment side effects and whether these are likely to last. Whatever the outlook, you and your partner may find it helps to discuss your concerns. You can find ways to be intimate during and after treatment. For some couples, it helps to talk with a sex counselor.
The Promise of Cancer Research
- Research on Prevention
- Research on Screening
- Research on Treatment
Doctors all over the country are conducting many types of clinical trials (research studies in which people volunteer to take part). They are studying new ways to prevent, detect, and treat prostate cancer.
Clinical trials are designed to answer important questions and to find out whether new approaches are safe and effective. Research already has led to many advances, and researchers continue to search for more effective methods for dealing with prostate cancer.
Men who join clinical trials may be among the first to benefit if a new approach is effective. And even if people in a trial do not benefit directly, they still make an important contribution by helping doctors learn more about prostate cancer and how to control it. Although clinical trials may pose some risks, researchers do all they can to protect their patients.
If you are interested in being part of a clinical trial, talk with your doctor.
Research on Prevention
Researchers are looking for ways to prevent prostate cancer:
- Diet: Some studies suggest that eating foods that have tomatoes in them may help protect men from prostate cancer. Lycopene is an antioxidant in tomatoes and some other fruits and vegetables. Research is in progress to see if lycopene can help prevent prostate cancer. A diet low in fat is also under study.
- Dietary supplements: The Selenium and Vitamin E Cancer Prevention Trial (SELECT) is studying these two supplements. The goal of the study is to learn whether these supplements can reduce the risk of developing prostate cancer.
- Drug: The Prostate Cancer Prevention Trial was a large study to test a drug that doctors thought might lower the risk of prostate cancer. The drug is finasteride. In the study, the drug did reduce the chance of developing prostate cancer. However, men who developed prostate cancer while taking the drug were more likely to have tumors that seemed to be high-grade. High-grade cancer grows and spreads more quickly than low-grade cancer. Researchers are now studying tumors from men in the study to see if they were really high-grade or only looked that way. If you are concerned about getting prostate cancer, you may want to talk with your doctor about the potential benefits and possible risks of taking finasteride. You also may consider taking part in another prostate cancer prevention trial.
Research on Screening
Researchers are studying ways to check for prostate cancer in men who have no symptoms. Screening can help find prostate cancer at an early stage. But studies have not shown whether screening saves lives. The Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial (PLCO) is designed to show if certain screening tests can reduce the number of deaths from these cancers. NCI supports this study. The prostate screening tests that PLCO is studying are the PSA test and digital rectal exam. Researchers will screen the men in the study until 2007. The trial will assess the harms and potential benefits of routine screening for prostate cancer. The results of this trial may change the way men are screened for prostate cancer.
Research on Treatment
Researchers are studying many types of treatment and their combinations:
Surgery: Different methods of surgery are being developed:- Robotic prostatectomy: The doctor uses a laparoscope and a surgical robot to help remove the prostate.
- Cryosurgery: Surgeons use a tool that freezes and kills prostate tissue in men with early prostate cancer.
- Radiation therapy: Doctors are studying different doses of radiation therapy. They are looking at the use of radioactive implants after external radiation. And they are combining radiation therapy with hormone therapy.
- Hormone therapy: Researchers are studying different schedules of hormone therapy.
- Biological therapy: Doctors are testing cancer vaccines that help the immune system kill cancer cells.
- Chemotherapy: Researchers are testing anticancer drugs and combining them with hormone therapy.
- Watchful Waiting: Men with early prostate cancer usually do not have any symptoms of disease. For these men, researchers are comparing having surgery or radiation right away against watchful waiting. Men in the watchful waiting group do not receive treatment until they have symptoms. The results of the study will help doctors know whether to treat early stage prostate cancer right away, or only if symptoms appear or get worse.
Researchers also are looking at ways to lessen the side effects of treatment, such as bone thinning and impotence.
National Cancer Institute Information Resources
You may want more information for yourself, your family, and your doctor. The following National Cancer Institute (NCI) services are available to help you.
Telephone
The NCI's Cancer Information Service (CIS) provides accurate, up-to-date information on cancer to patients and their families, health professionals, and the general public. Information Specialists translate the latest scientific information into understandable language and respond in English, Spanish, or on TTY equipment. Calls to the CIS are free.
- Telephone: 1-800-4-CANCER (1-800-422-6237)
- TTY: 1-800-332-8615
